When you buy through our links, we may earn a commission. Products or services may be offered by an affiliated entity. Learn more.
Bedroom Environment: What Elements Are Important?
A relaxing environment is essential for a good night’s rest. Studies have shown people simply sleep better when their bedroom is optimized for temperature, noise and light levels, and comfort. And since sleep quality and duration are directly tied to other aspects of human health, a bedroom environment that promotes sleep can also improve how you feel while you’re awake.
Best of all, creating the ideal bedroom doesn’t need to break the bank. There are several cost-effective ways to make your sleep space more soothing and suited for rest.
Looking to improve your sleep? Try upgrading your mattress.
Temperature
Some people run hot in bed while others sleep somewhat cool. However, any healthy adult will experience a drop in body temperature while they sleep. This naturally occurs during the initial stages of your sleep cycle because a lower core temperature makes you feel sleepy, whereas a higher temperature helps you stay alert during the day.
Whether you only use a top sheet or sleep beneath a thick comforter, many experts agree the ideal bedroom temperature for sleeping is 65 degrees Fahrenheit (18.3 degrees Celsius). This might sound a bit chilly for some, but a cooler thermostat setting helps you maintain a lower core temperature while you sleep.
That said, 65 degrees may not be the best temperature for everyone. If you find this setting too cold, try adding a layer or two to your bedding. If you’re too warm or the weather is particularly hot or humid, consider removing a layer or wearing lighter bedclothes in order to stay cool in bed.
Noise
It should come as no surprise that a quieter bedroom is better for sleep than a louder one. Loud noise disturbances can cause severe sleep fragmentation and disruption, which in turn can have negative impacts on your physical and mental health. Research even suggests that noise at low levels can cause you to shift to a lighter sleep stage or wake up momentarily.
You should strive to keep your bedroom as quiet as possible by blocking outside noises. The whir of a fan or a soothing white noise machine can effectively mask other sounds and help you fall asleep. Some people also enjoy listening to music when they go to bed. Ambient sounds or soothing music, which may also alleviate anxiety and ease physical pain. Noise-blocking curtains are also widely available.
Light
The circadian rhythms that guide your sleep-wake cycle are heavily influenced by natural light and darkness. During the day, your eyes perceive sunlight and signal the brain to produce cortisol, a hormone that helps you stay alert and energized. At night when darkness falls, your brain then produces another hormone, melatonin, to induce feelings of sleepiness and relaxation.
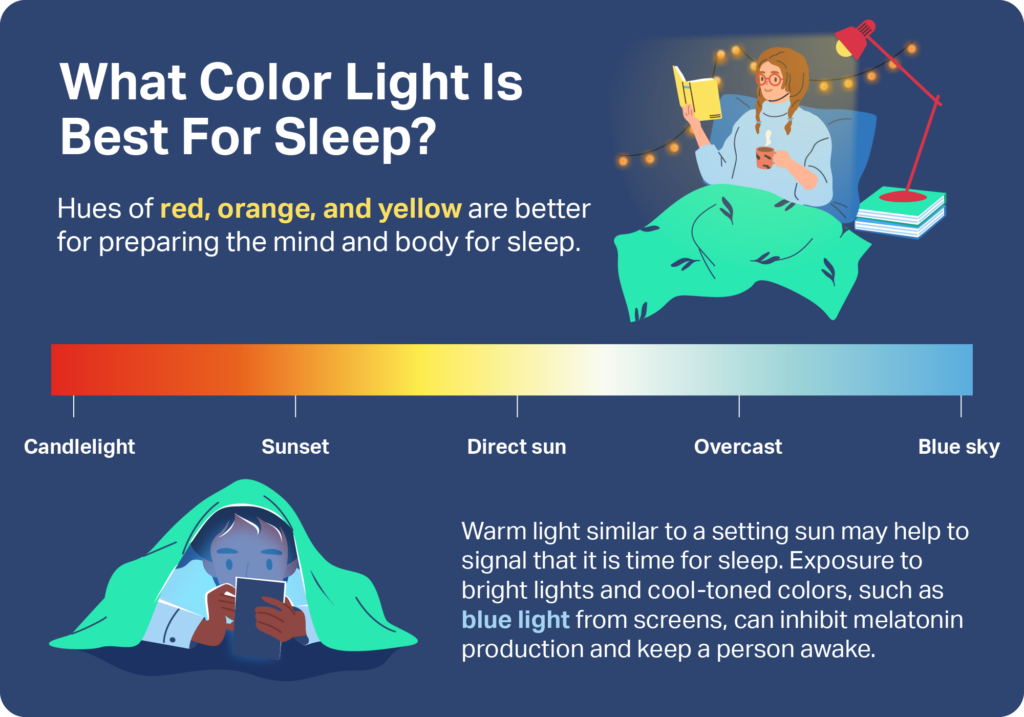

Exposure to artificial light in the evening can delay circadian rhythms and prolong sleep onset, or the time it takes you to fall asleep. Light intensity is measured in units known as lux. Studies have found that exposure to light sources with a lux of 10 or higher later in the day can lead to more nocturnal awakenings and less slow-wave sleep, a portion of your sleep cycle that is vital to cell repair and bodily restoration. Smartphones, televisions, and other devices with screens also produce artificial blue light that can be detrimental to sleep, even if you use dimmer “nighttime” screen settings.
Keep your bedroom light levels as low as possible if you like to read in bed before sleep. Dimmer lights will help you fall asleep more easily. Another good rule-of-thumb is to avoid using screen devices – including televisions – in your bedroom.
Mattress and Bedding
Depending on your sleep preferences, you may enjoy the close body contour of memory foam, the gentle support of latex, or the springy feel of a mattress with coils. Some studies have found that a newer mattress will promote better sleep quality and alleviate more back pain than an older model. However, the best mattress for you likely depends on individual factors like body weight, normal sleep position, and whether you prefer lying on a soft or firm surface.
You should also choose your bedding items based on personal criteria. Important considerations for selecting the best pillow include firmness, loft (thickness), and durability. For sheets, the best option for you may come down to whether you prefer a crisp or silky hand-feel and how hot you sleep at night.
A sanitary bedroom is also important for promoting healthy sleep. Vacuuming your carpet and regularly washing your bedding can reduce the presence of dust mites, small arthropods that trigger allergies. Just be sure to follow washing and drying instructions on your bedding’s care tags to avoid damage or excessive shrinkage.
Additional Tips for a Relaxing Bedroom
To ensure your bedroom is a relaxing environment that promotes healthy sleep, you should take steps to improve your surroundings.
Many experts agree you should wash your sheets at least once every two weeks. If you sweat excessively in your sleep or share your bed with a pet, you may want to consider weekly cleanings. Routine washings not only prevent dust mites and body oils from building up but can also promote better sleep.
Certain scents can help you feel more relaxed. For example, some studies have found lavender essential oil can improve sleep quality and allow you to wake up feeling more refreshed. Other fragrances, such as peppermint and heliotropin, may also be effective. If you share your bed with a partner, their unique scent may also help you sleep better.

Still have questions? Ask our community!
Join our Sleep Care Community — a trusted hub of sleep health professionals, product specialists, and people just like you. Whether you need expert sleep advice for your insomnia or you’re searching for the perfect mattress, we’ve got you covered. Get personalized guidance from the experts who know sleep best.
References
13 Sources
-
National Institute of Neurological Disorders and Stroke. (2022, September 26). Brain basics: Understanding sleep.
https://www.ninds.nih.gov/health-information/public-education/brain-basics/brain-basics-understanding-sleep -
Harding, E., Franks, N., & Wisden, W. (2019). The Temperature Dependence of Sleep. Frontiers in Neuroscience, 13.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6491889/ -
Improve Sleep: Tips to Improve Your Sleep When Times Are Tough. CDC. (2020, September 22).
https://blogs.cdc.gov/niosh-science-blog/2020/06/29/sleep-hwd/ -
Hume, K., Brink, M., & Basner, M. (2012). Effects of environmental noise on sleep. Noise & Health: A Bimonthly Inter-Disciplinary International Journal, 14(61), 297–302.
https://pubmed.ncbi.nlm.nih.gov/23257581/ -
Trahan, T., Durant, S., Müllensiefen, D., & Williamson, V. (2018). The music that helps people sleep and the reasons they believe it works: A mixed methods analysis of online survey reports. PLoS One, 13(11).
https://pubmed.ncbi.nlm.nih.gov/30427881/ -
Blume, C., Garbazza, C., & Spitschan, M. (2019). Effects of light on human circadian rhythms, sleep and mood. Somnologie, 23(3), 147–156.
https://pubmed.ncbi.nlm.nih.gov/31534436/ -
Tosini, G., Ferguson, I., & Tsubota, K. (2016). Effects of blue light on the circadian system and eye physiology. Molecular Vision: Biology and Genetics in Vision Research, 22, 61–72.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4734149/ -
Jacobson, B. H., Boolani, A., & Smith, D. B. (2009). Changes in back pain, sleep quality, and perceived stress after introduction of new bedding systems. Journal of Chiropractic Medicine, 8(1), 1–8.
https://pubmed.ncbi.nlm.nih.gov/19646380/ -
National Institute of Environmental Health Sciences. (2001, August 6). Study Shows Simple Steps Can Reduce Dust Mite Allergens in Bedrooms.
https://www.niehs.nih.gov/news/newsroom/releases/2001/august06/index.cfm -
Krouse, L. (2019, November 19). How Often Should You Really Wash Your Sheets? Experts Share the Magic Number. Prevention.
https://www.prevention.com/health/a29824369/how-often-should-you-wash-your-sheets/ -
Lillehei, A. S., Halcón, L. L., Savik, K., & Reis, R. (2015). Effect of Inhaled Lavender and Sleep Hygiene on Self-Reported Sleep Issues: A Randomized Controlled Trial. Journal of Alternative and Complementary Medicine, 21(7), 430–438.
https://pubmed.ncbi.nlm.nih.gov/26133206/ -
Sowndhararajan, K., & Kim, S. (2016). Influence of Fragrances on Human Psychophysiological Activity: With Special Reference to Human Electroencephalographic Response. Scientia Pharmaceutica, 84(4), 724–752.
https://pubmed.ncbi.nlm.nih.gov/27916830/ -
Hofer, M., & Chen, F. (2020). The Scent of a Good Night’s Sleep: Olfactory Cues of a Romantic Partner Improve Sleep Efficiency. Psychological Science, 31(4), 449–459.
http://journals.sagepub.com/doi/10.1177/0956797620905615




















